The Fast Facts
- Generally, the patient experiences a lot of pain after the treatment, even if the treatment involves only medicines or surgery.
- A genetic mutation has been detected in the cationic trypsinogen gene that causes acute pancreatitis in 80% of its carriers.
- Due to released enzyme by necrosed pancreatic cells it remains as one of the core diagnostic criteria in acute pancreatitis.

Before going into the nutritional management of acute pancreatitis, let’s know in nutshell about its factor, symptoms, complications etc.
The pancreas is protected in contradiction of its own enzyme by their synthesis as proenzymes. Acute pancreatitis occurs when activated pancreatic enzymes (activated prematurely in pancreas) are generated within the pancreatic system.
The clinical feature of pancreatitis results from auto digestion of tissue and toxic effects of digestion products like serum and urinary amylase concentration. Due to released enzyme by necrosed pancreatic cells it remains as one of the core diagnostic criteria in acute pancreatitis.
The severity of pancreatitis can be seen by the Ranson’s criteria to classify pancreatitis.
What Can Cause Acute Pancreatitis?
The main cause of acute pancreatitis are:
Gallstones: This condition is seen in about 40% of cases. Although it is not entirely clear how this occurs. The stones block the pancreatic duct, causing damage to the enzyme-forming process. Due to this, there is a risk of tissue damage in this organ.
Alcohol: It is seen in about 30% of cases. Systematically drinking alcohol, regardless of its amount, leads to chronic pancreatitis after a few years. However this does not happen in all drinkers. Other health factors also cause its emergence.
Second Factor: A genetic mutation has been detected in the cationic trypsinogen gene that causes acute pancreatitis in 80% of its carriers. By ERCP (endoscopic retrograde cholangio pancreatography) procedure, doctors try to find out the problem.
Other Factors:
| Direct | Indirect |
| Sudden immune attacks in the pancreas
Damage of pancreas or gallbladder from surgery or injury Excess triglycerides in blood | Kawasaki Disease
Viral and bacterial infections like mumps and mycoplasma |
| Footnote. There are many etiology factors that cause acute pancreatitis like gallstone, alcohol, genetic mutation and other direct and indirect factors as mentioned above. |
Signs and Symptoms of Acute Pancreatitis.
The symptoms of pancreatitis includes:
- Constant or intermittent pain of fluctuating intensity in the upper abdominal region that radiates to the back. Symptoms worsen with ingestion of food.
- Swollen and tender abdomen.
- Nausea and vomiting which are precipitated by large meal and alcohol consumption.
- Steatorrhoea and malabsorption.
- Mild jaundice, sweating, rapid pulse, fever are also seen.
| Footnote. There are many symptoms like nausea and vomiting, sweating, fever and many more. |
Complications.
Some of its complications include low blood pressure, heart failure, kidney failure, diabetes, ascites and cysts in pancreas.
| Footnote. Complications like low blood pressure, heart failure etc. |
How to Diagnose Acute Pancreatitis?
Acute pancreatitis is diagnosed through blood test. This test shows whether the pancreas and lipases are leaking out from the pancreas into the bloodstream. Thereafter, the doctor recommends the patient for an ultrasound, CT scan or MRI scan. These tests are considered as very important for the further treatment.
After the diagnosis, the patient get admitted to the hospital. Intravenous feeding are started like saline and fluids. Medications are also given for pain and infection.
If the problems are increased, doctors recommend surgical procedures. This procedure is follow to expel fluid from the organ, repair tissue damage from injuries or open blocked ducts or perform any surgery if required.
Generally, the patient experiences a lot of pain after the treatment, even if the treatment involves only medicines or surgery. However, several medicines are prescribed to the patient to deal with pain.
Acute pancreatitis can be related to diabetes, as people suffering from it often prone to the disease.
| Footnote. It is diagnose by blood test. After that doctor takes decision. According to the patient’s condition doctor takes steps how to treat it. |
Who are Eligible for Treatment?
If the condition of the patient are not improved, they need treatment. However, the form of treatment differs from one patient to another. If medicines alone are sufficient to alleviate the symptoms, then no more further treatment required. If the disease is not cured by drugs, then a surgery is required.
| Footnote. According to the patient’s condition treatment are done. If medicines are working then no further actions are needed, but if not surgery may require. |
Nutritional Management or Support in Acute Pancreatitis.
Acute pancreatitis is frequently understood in a catabolic state, characterized by profound metabolic, cardiovascular, pulmonary, hemodynamic, hematological and renal aberrations.
Metabolic support and parenteral nutrition becomes vital in order to reduce mortality. Since TPN (Total Parental Nutrition) feeding needs specialized set up and are expensive and needs long term maintenance. Therefore, it is difficult for patients to bear the expenses.(1),(2),(3),(4)
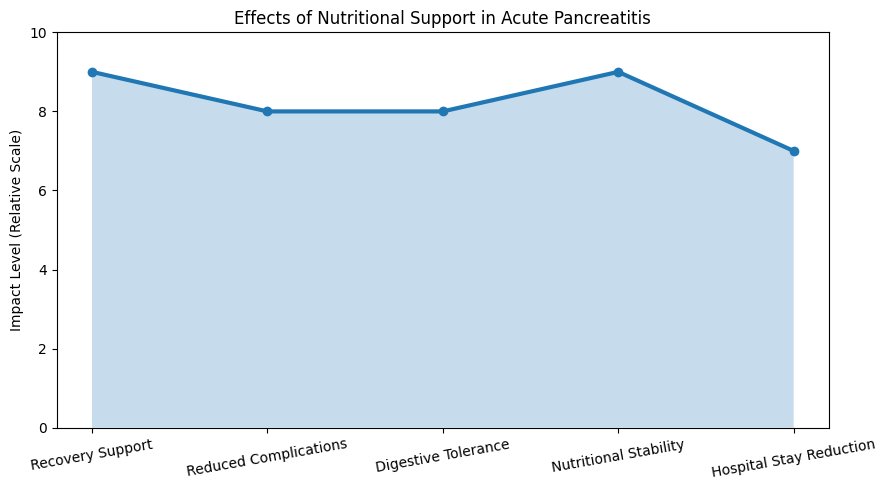
Hence, enteral nutrition is a mostly preferred. This type of feeding is safe and accepted with less infections/non – infectious complications. The nutritional management goals of acute pancreatitis include:
- Give rest to pancreas by maintaining fluid balance.
- No food by mouth should be given till the pain and fever reduce, as the oral intake can further exaggerates the symptoms by an increased secretory mechanism of pancreatic enzyme and bile.
- The patient needs to be supported by early enteral nutrition with the formulation of nutrient in predigested forms and supplementation with low fat intake to prevent further precipitation of malnutrition. Sometimes TPN is required.
- After oral feeding is resorted then go for clear liquid diet with a waiting period. Then see the response of the patient whether they are coping with it or not.
- A low fat diet with an intake of total fat-30g/day should be consumed. According to patient’s tolerance consumption may be increase. MCT (Medium Chain Triglycerides) may be incorporated for better digestibility and assimilation, as they do not require the pancreatic enzyme system for the same. MCT helps in increasing the total caloric intake of the patient.
- A strict monitoring of all the biochemical parameters starting from enzymic assay to serum albumin concentration should be done and checked on regular basis.
- Decreased in calcium levels often seen during acute pancreatitis. This can be due to (i) Hypoalbuminemia (as calcium is bound to protein) and (ii) soap formation of calcium with fatty acids created by fat necrosis. Hence, calcium supplementation may be required.
| Footnote. Acute Pancreatitis is often characterized by catabolic state. According to patient’s condition management in nutrition are required. Sometimes due to malnutrition TPN are administrated. It is recommended to go for low fat diet. |
Bottom Line.
Acute Pancreatitis is one of the serious short term pain. If untreated and not diagnosed properly it can be chronic and severe. Excess smoking and consumption of alcohol should be avoid.
According to patients condition treatments are required.
A proper nutritional management guidelines of acute pancreatitis needs to look after. It is recommended to start with low fat diet which helps pancreas to heal, before going back to normal diet.
It would be better always to eat healthy balanced diet. Include some physical activity like yoga or exercise to maintain a healthy lifestyle.
+4 Sources
Freaktofit has strict sourcing guidelines and relies on peer-reviewed studies, educational research institutes, and medical organizations. We avoid using tertiary references. You can learn more about how we ensure our content is accurate and up-to-date by reading our editorial policy.
- Enteral versus parenteral nutrition for acute pancreatitis; https://pmc.ncbi.nlm.nih.gov/articles/PMC7120370/
- Nutrition management in acute pancreatitis: Clinical practice consideration; https://pmc.ncbi.nlm.nih.gov/articles/PMC7211526/
- A prospective, randomized trial of clear liquids versus low-fat solid diet as the initial meal in mild acute pancreatitis; https://pubmed.ncbi.nlm.nih.gov/17613280/
- Efficacy of early oral refeeding in patients of mild acute pancreatitis; https://pmc.ncbi.nlm.nih.gov/articles/PMC5648961/










































 Workout
Workout

 Meditation
Meditation



 Podcast
Podcast
 E-book
E-book