The Fast Facts
- People have to depend on protein to keep away from muscle wasting, but avoid the situation of overloading a lot of protein on your kidneys at the same time.
- They would, in other words, have to eat, on a daily basis, 86 – 90 large lettuce with a low content of potassium and sodium.
- It also motivates you to follow the food plan, teaches you to switch to a social diet, manage symptoms, and so on.

Adjusting your diet to support kidney health is a vital part of coping with kidney failure. Although making changes in diet can be difficult, they can also be helpful in slowing down the disease and reducing the complications.
This article takes readers on a journey through kidney functions, their failure, and what they should eat. It also motivates you to follow the food plan, teaches you to switch to a social diet, manage symptoms, and so on. Here is a good starting point.
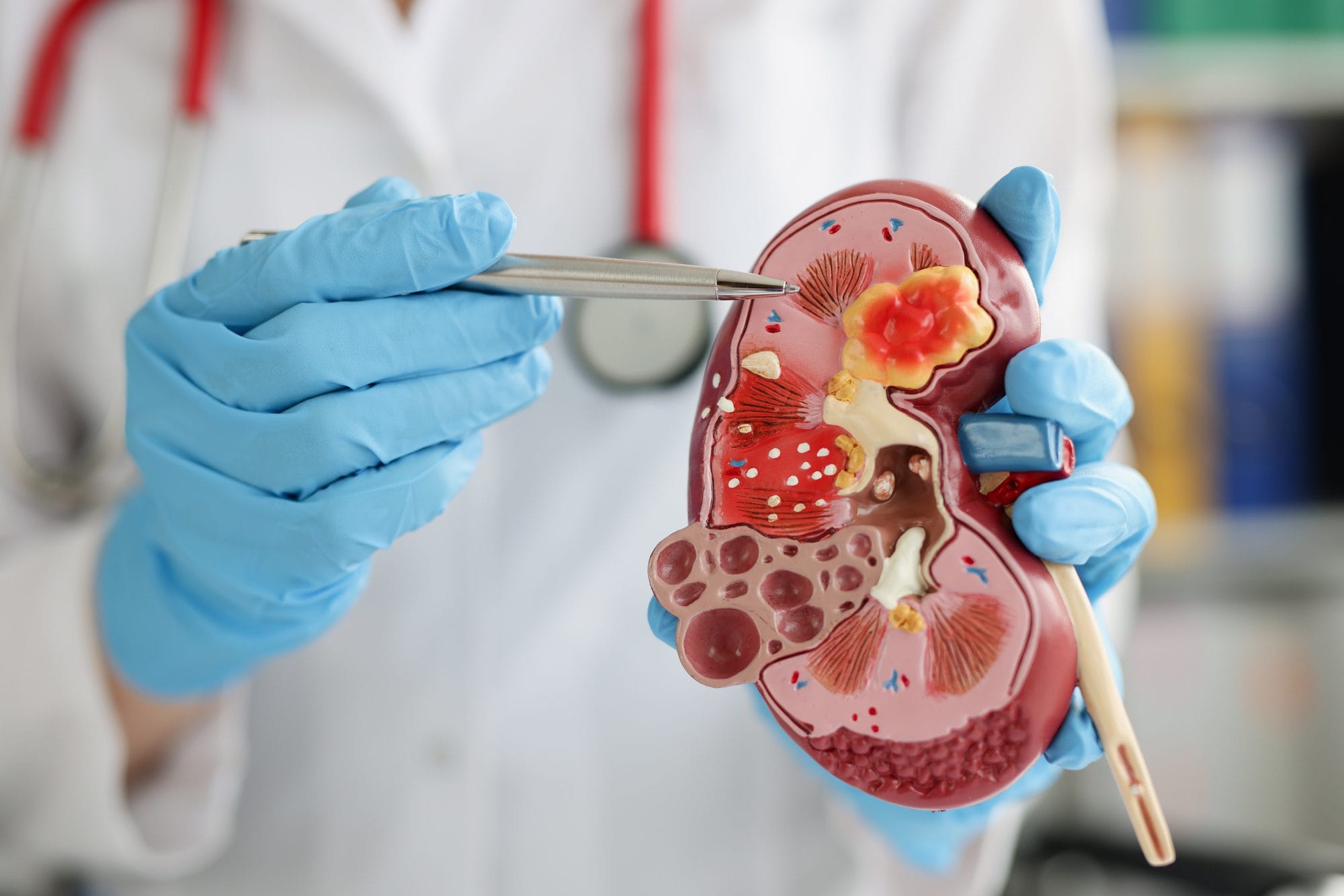
Understanding Kidney Failure And Its Nutritional Implications.
By eliminating wastes and holding essential substances, the kidneys work as blood purifiers. In end stage kidney failure there is a cessation of this process. This allows for the buildup of waste matter and the retention of potassium and phosphorous minerals at high levels.
Once this is managed through diet, it is a life saver indeed. Nutritional needs will definitely get adjusted with the different point where the kidneys are. Cutting down on your protein, sodium, and phosphorous intake in the early stages will greatly slow down the progress of the disease.

Core Nutritional Principles for Kidney Failure.
1 Protein.
People have to depend on protein to keep away from muscle wasting, but avoid the situation of overloading a lot of protein on your kidneys at the same time. Getting plant-based proteins like beans, lentils, and of course, tofu apart from good fiber is obviously one of the best ways to get proteins without meats. Additionally, eggs, skinless poultry, and fish are all fine examples of low-fat animal protein sources. However, with fish and seafood, make sure it is in the lean portion.
Protein requirement varies from person to person, depending on their health, nutritional status, and body size. To determine your specific needs, consult with a dietitian; these needs generally fall between 0.6 to 0.8 grams of protein per kilogram of body weight. There is also a role for amino acid supplements that are timed around your exercise.
2 Phosphorus.
Phosphorus has the primary function together with calcium in maintaining bone health. In cases of kidney disease, excessive phosphorus builds up as the subconscious process gets disrupted. The food categories generally high in phosphorus are: dairy products, beans, lentils, nuts, and whole grains. Also, processed meats and sodas belong to this group.
Phosphorus and beans are a part of your meals but with a little effort applied to the preparation. You can remove some of the extras by soaking highly phosphorous beans and grains. The reason of doing this extraction can be to apply fresh dairy or meet food alone. Phosphate binders can be accompanied by the already prescribed meal where the drug prevents the absorption of phosphorus through the intestines. This is in case you are not able to work through your diet needs alone.
3 Potassium.
Potassium helps the proper function of nerves and muscles, but it is one of the substances that accumulate during kidney failure. Thus, you need to manage your intake of bananas, potatoes, tomatoes, and all other potassium-rich foods when you are dealing with a kidney problem.
What you can do is look for food labels. Among the mentioned examples, plantain and cauliflower carry less potassium as compared to oranges and broccoli.
It would be better if you change your focus to potassium-poor fruit such as berries, apples, and melon as well as less watery vegetables. The lower potassium
Here is an example of a potassium-controlled diet that includes vegetables: green beans, small lymph nodes (dilutes boiled vegetables in a large amount of water),
0 mg a day as a rough estimate, which is nearly the same low limit of 86 mg. They would, in other words, have to eat, on a daily basis, 86 – 90 large lettuce with a low content of potassium and sodium. Note that a 0mg end-point is impossible by the logical context but asks for creativity in this argument.
4 Sodium.
Sodium is a mineral which causes our body to hold water and kidney impairment as you may already know is associated with a more rapid and severe progression of heart and kidney disease. You should get rid of table salt as much as possible and never put more than a pinch of it over your dish. Avoid using high sodium drugs like garlic salt, stock cubes, or soy sauce when cooking, as these are concentrated sources of sodium. Opt for fresh foods rather than canned or processed products and avoid buying them from the nearest fast-food store, as it is unlikely that a restaurant staff will provide you with an accurate list of ingredients used for their meals. The latter means that you are in control of selecting your pockets of ingredients that are lower in sodium than any of the shelf-stable or frozen ones.
It is always good to see your local pharmacist regularly not only as a courtesy to him/her but also to get as much information about your health as you can during such appointments.
Also, request that the pharmacist reviews all your medications with hidden sodium content, so you know which ones to avoid.
In fact, the question about whether the patient’s dietary intake would be the only way to receive his/her needs should also be examined. The patient should, therefore, weigh the benefits and downsides of such a diet at a conference on health care with the doctor.
5 Fluids.
Always maintaining the right amount of fluids in your body could save you from kidney overload and keep you hydrated, unlike dehydration that will knock you out. Hence, thirst, which is a sign that you are low in fluids, should trigger the intake of water.
On the contrary, the development of swelling may show that you are retaining excess water. The main sources of fluid intake are drinking fluids and eating foods rich in water – such as fruits and vegetables.
It should be noted that your daily fluid intake may be less or more, so let’s have a record of your input. To balance your daily consumption and excretion, the daily procedure of your weight, as well as the measurements of the swollen feet, is a good indicator. Measure your intake and remember that your daily fluid intake needs can vary. A general guideline is about four to five cups, but this can change based on your individual health condition and any medical advice you receive.
Nutritional Supplements For Kidney Failure: Benefits And Risks.
Once you have reduced nutrient absorption, and are having trouble absorbing vitamins and minerals, taking dietary supplements is a must to combat the deficiencies.
Firstly, the heart, bones, and blood of the human body benefit from Vitamin D and omega-3s. In addition, psyllium, a soluble fiber, can be beneficial, too. A notable risk of vitamin A supplementation is the excessive amount of it that could lead to toxicity, particularly in the case of kidney failure.
Besides, herbal remedies might result in drug interactions. Therefore, consulting your doctor first is indispensable.
The doctor can look at the patient’s symptoms and decide on the added supplementation, or the doctor may do lab work to see if deficiencies still persist; if so, he/she may give the patient some targeted supplements under strict observation.
Mostly, the doctor may perform a repeatable test after a few months, to confirm if the patient has adequate but not massive levels of nutrients from medication. Therefore, carefully selecting only beneficial and safe supplements is a crucial part of the treatment plan.
That is how you characterize nutritional supplements for kidney failure, which is their effectiveness, and when and how to start the administration.
Practical Tips For Meal Planning And Preparation.
Hacking delicious and kidney-friendly meals is a piece of cake once you go for a well-organized approach since it will help you to keep the positive emotional circle, that is, feel less deprived of the loved products that can be avoided while being sick.
From our experience, yes! Who would have thought that eating healthily would lead to something exciting? This still can happen, using cookbooks and websites where you can find meals that suit the kidneys, and the link will tell you more about unique detox recipes.
To make your meals more exciting, you can also create fresh, more palatable ones by using alternative versions of allergenic products, hence still enjoy your food. Registered dietitians are health professionals who work with individuals to develop personalized dietary plans and help them to satisfy their nutritional needs.
Managing Common Challenges And Concerns.
1 Social Situations and Dining Out.
Let your family members who cook for you know what your dietary restrictions are. Review ingredients lists and offer, if possible, a kidney-friendly dish to take along.
Before going to a restaurant, call in advance, and enquire about sodium levels and the possibility of modifying a particular dish.
Visit the sites of the kidney organizations that detail those restaurants that are friendly to kidney diseases. There are some nutrition apps that help you to look at the restaurant’s food before going there.
Locating good food while traveling may be a headache as well.
Carry some snacks that go well with the kidney, and check hotel restaurants’ menus before the trip. Ask for a fridge that is small, and you can use it to preserve your food. Shelves of airports and planes are stoking furore with more options of meals for kidney patients.
2 Recurring Symptoms of Kidney Failure.
Changes in your appetite are not a strange feature of kidney disease. In the presence of nausea, the situation can be worse but hope is not lost. This can be solved by sipping fluids and eating controlled foods during meals. You will manage better when you eat fewer, but more regular meals.
In case you feel full after a small amount of food, take nutritional supplements, for example, an energy-laden beverage could be suitable.
If changes to your diet do not alleviate bowel problems like constipation or diarrhea, you should consult a doctor and receive proper medication. In case of constipation, include more soluble fiber and limit the intake of gas-producing foods.
For diarrhea, be ready for a BRAT diet in case your general practitioner tells you to increase the dosage. Further, a little bit of physical activity also can ease off fatigue.
3 Emotional and Psychological Support.
This kidney diet is a radical change in life. Societalizing with kidney health communities for mutual advice and encouragement can be a significant help. You can think of seeking psychological support from a therapist who is skilled at handling chronic diseases.
Besides, your healthcare provider’s team probably has resources available to reduce stress. The meditation, writing diary, or mild exercise are some of the ways of self-care.
Give yourself some slack; there is no need for perfection. One meal at a time, please.
Frequently Asked Questions.
1 What foods should I completely avoid if I have kidney failure?
People with kidney failure should avoid foods high in potassium (like bananas, oranges, tomatoes), high-phosphorus foods (like dairy, chocolate, nuts), and high-sodium items (fast food, canned foods, pickles). Processed meats are also best avoided.
2 Can I eat fruits if I have kidney failure? Which ones are safe?
Yes, you can eat fruits, but you must choose low-potassium fruits such as apples, berries, grapes, pineapple, and watermelon. High-potassium fruits like bananas, oranges, and avocados should be limited.
3 How much protein should a kidney patient eat per day?
Protein intake depends on kidney stage, but generally 0.6–0.8 g per kg of body weight is recommended. Kidney patients should prefer plant-based proteins and lean options like fish, eggs, and skinless chicken. A dietitian can personalize the exact amount.
4 Is drinking too much water harmful for kidney failure patients?
Yes. Some kidney failure patients need restricted fluids, especially if swelling, shortness of breath, or low urine output occur. Most people are advised around 4–5 cups per day, but it varies. Always follow your doctor’s fluid limit.
5 Can kidney failure be improved or slowed down with diet alone?
Diet cannot reverse kidney failure, but it can slow down progression, reduce symptoms, and lower waste buildup. Controlling protein, sodium, potassium, and phosphorus helps protect remaining kidney function and improves quality of life.
Bottom Line.
By eating the proper, nutritious food for kidney health, you can maintain perfect phosphorus, potassium, and sodium levels and provide your kidneys the opportunity to function at an optimal level. Always support with fresh, whole foods that are tailored to your new situation. Every aspect, from meal plans to community connections is available for your support. What you do matters; therefore take the pledge of embarking on the path to kidney health.












































 Workout
Workout

 Meditation
Meditation



 Podcast
Podcast
 E-book
E-book