The Fast Facts
- Its role is to alter the shape of the lens through movement of the ciliary muscle — allowing us to focus on near objects — and also to make the fluid (the aqueous humour) which circulates in the chamber between the lens and the inner surface of the cornea.
- The products of this inflammation in the ciliary body and iris may become visible as a welling up of pus-like material in the front chamber of the eye between the lens and the cornea.
- The uvea is the name given to the area that is comprised of three distinct structures located in the center of the eyeball.

The uvea is the name given to the area that is comprised of three distinct structures located in the center of the eyeball. These structures are so intimately connected that disease or inflammation in one region will quickly spread to another.
Many diseases like syphilis, tuberculosis and even rheumatoid arthritis can affect the uvea, though serious damage is rare. Luckily, inflammation in this area responds quickly to treatment.
What is the Uveal Tract?
This area of the eye is made of three specialized parts: the choroid, the ciliary body and the iris of the eye. The choroid is a thin sheet of membrane between the outer protective sclera and the retina. This membrane is full of blood vessels which supply the retina and form an intricate lattice throughout most of the eye.
In this lattice there are supporting tissues which contain a varying amount of pigment: this prevents light bouncing around the back of the eye giving confusing images.
The ciliary body consists of a ridged-up area of the uveal tract right at the front of the eye. Its role is to alter the shape of the lens through movement of the ciliary muscle — allowing us to focus on near objects — and also to make the fluid (the aqueous humour) which circulates in the chamber between the lens and the inner surface of the cornea.
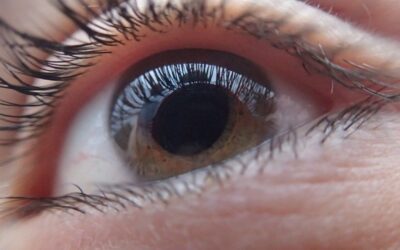
Attached to the ciliary body is the third specialized area, the iris. This is the part of the eye whose pigment gives the eye its colour. It acts like the aperture stop of a camera, its muscle fibres dilating or contracting the pupil and thus controlling the light reaching the retina.
Uveal Tract Problems.
There are a number of conditions that can affect the uveal tract ranging from defects in development to infection.
Abnormalities.
This might be present from birth: for example, part of the iris of the eye may be missing or its pigment may be incomplete. These defects do not usually matter unless the missing portion is large enough to affect its function.
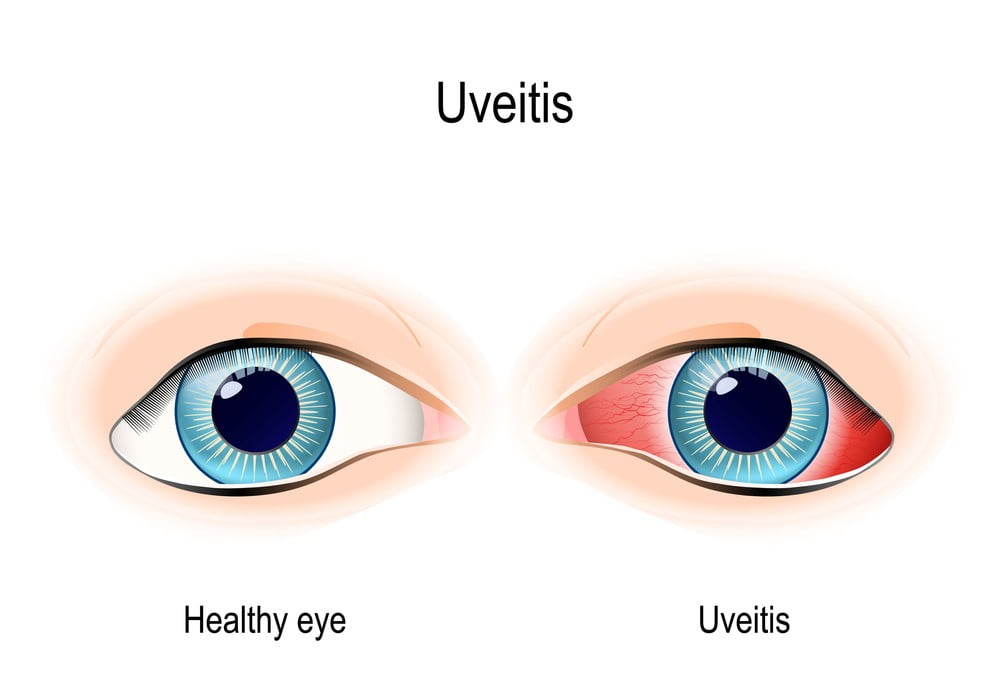
Uveitis.
It is a general term that is used to describe various inflammations of the uvea. The causes of this condition include both bacteria and viruses which may infect the uvea.
Other conditions can produce inflammation through changes in the body’s immune system. Bacterial infections rarely cause inflammation in the front part of the uvea, but are more common in the choroid membrane. The symptoms of uveitis depend on whether the iris or the choroid are involved.
Iritis.
It produces a red painful eye; vision may be blurred and the eye may have a watery look. The redness comes about from engorgement of the blood vessels from near the iris in the neighbouring sclera white of the eye. The swollen iris and ciliary body, and spasm of the muscles in the ciliary body cause pain.
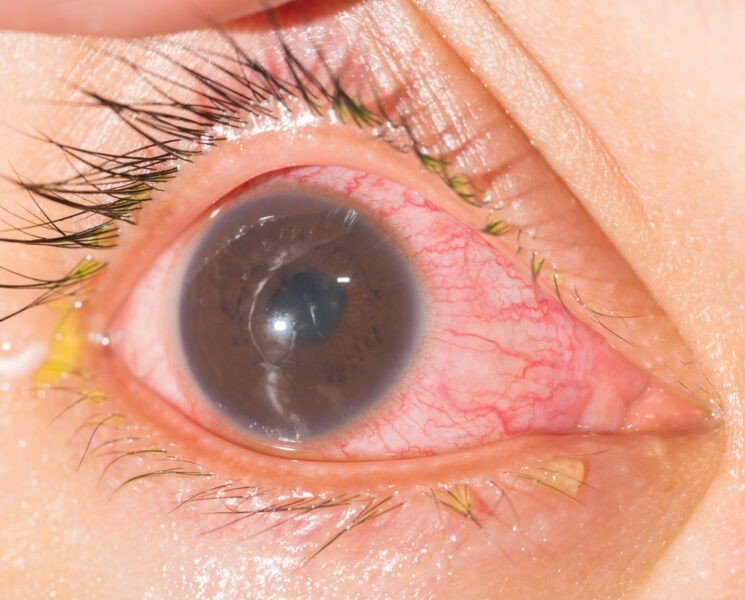
The products of this inflammation in the ciliary body and iris may become visible as a welling up of pus-like material in the front chamber of the eye between the lens and the cornea. Since strong light stimulates the tender ciliary muscles, a person with iritis tries to avoid light, often by keeping his eyes shut.
This unpleasant condition is treated by means of antibiotics or steroid drugs placed as drops into the eye to reduce the swelling. Drugs are also ‘dropped’ into the eye to paralyze temporarily the ciliary muscles to ease the pain and prevent the occurrence of adhesions affecting the central part of the lens.
| Read Now: 17 Super Food for Macular Degeneration |
Choroiditis.
It produces a gradual impair vision. The eyes may look normal, but a doctor using an ophthalmoscope will see patches of white scars on inner surface of the eye, often with black edges where the pigments have been disrupted by inflammation.
As with iritis, many of the inflammations of the choroid are caused by changes in the body’s immune system which produce this destructive process.
Various infections can also produce choroiditis, including toxoplasmosis which is caught from infected animals or undercooked food.
Glaucoma.
It is another problem that can occur in the front of the uvea. Here the delicate channels which drain off the fluid of the front of the eye become blocked, either because of thickening of the blood vessels or after attacks of iritis.
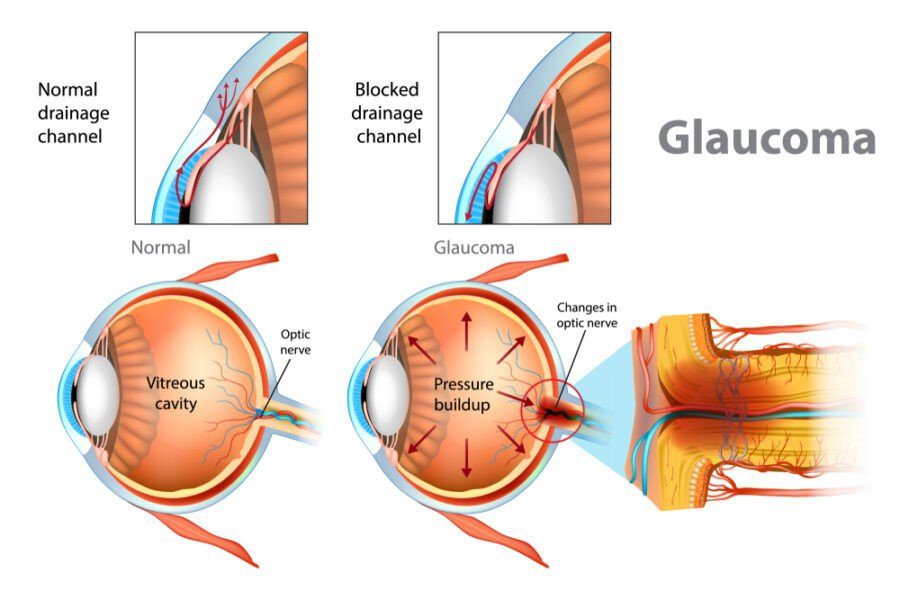
The fluid can no longer drain properly, so the pressure goes up and presses backwards against the retina, whose nerve fibres can become seriously damaged.
The condition is treated either with drugs — which lower the pressure by reducing the amount of fluid produced or by operations to improve drainage.
| Read Now: How To Take Care of Your Eyes Properly? |
Treatment.
Treatment of infections of the uveal tract involves administering drugs as eye drops. This reduces swelling and eases pain.
In most cases, uveitis is treated with certain types of eye drops. However, if it is caused by another internal disease, then the treatment of the disease which caused uveitis is started first and then the treatment for uveitis is done.
The main goal of treating uveitis is to reduce inflammation and redness in the eye. In some other cases, uveitis is treated according to its type:
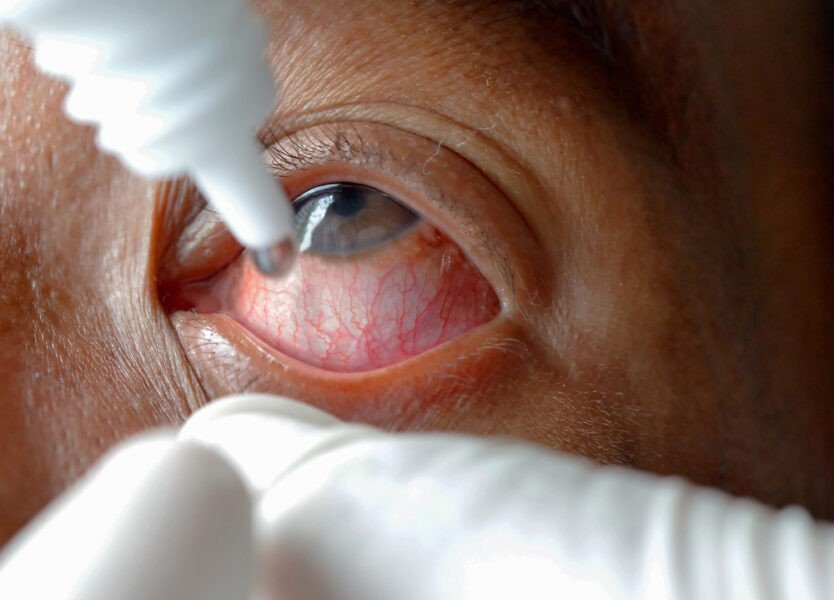
- In the treatment of anterior uveitis or iritis, some types of steroid eye drops are mainly used.
- Some steroid drugs are mainly used to treat postpartum uveitis. These medicines are either given as food tablets or injected, which is applied around the eye.
- In cases of infection or autoimmune diseases, the patient can be referred to another specialist doctor. Infection is cured with antibiotics or anti-viral drugs.
- Steroid drugs are used to treat intermediate uveitis. These medicines come in the form of food tablets, injections and eye drops. Some other painkillers may also be given to ease the pain.
Frequently Asked Questions.
Both these conditions cause pain and redness in the eye. Conjunctivitis, however, is an inflammation of the thin lining of the eyelids and white part of the eye, giving an itchy irritation of this whole area. In iritis, only the coloured area— the iris — becomes red, and the pain is like throbbing nature.
It is not common, but it does occur. It is usually caused by an uveal infection called toxoplasmosis. This attacks the thin membranous sheet between the sclera and the retina. Quite how people acquire this infection is not fully understood, but the parasite that causes it is widespread in dogs and cats, and can also be found in undercooked food. The condition responds well to treatment.
In glaucoma there is an obstruction at the drainage points that allow the fluid— called the aqueous humour — to drain away. The purpose of the drops is to keep free the point at which the fluid apes. It does this by tightening up the muscles that constrict the iris. When the iris is constricted like this, it is often difficult to focus in the distance, or in dim light.
Yes, this can happen, though quite why remains a mystery. But the risk of the iritis occurring is real enough for a damaged eye to be removed rather than risk the health of the other eye.
If the inflammation is caused by bacteria then only the doctor prescribe antibiotics. The antibiotics that are commonly given are:
Durezol.
Dexamethasone.
Mycophenolate Mofetil
Homatropin.
Ozurdex.
Apart from these medicines, doctor may prescribe different one as per the condition.
Bottom Line.
Inflammation between the outer layer of the eye and the retina at the back is the uvea, the central body of the eye which can be affected by disease and infection.
+5 Sources
Freaktofit has strict sourcing guidelines and relies on peer-reviewed studies, educational research institutes, and medical organizations. We avoid using tertiary references. You can learn more about how we ensure our content is accurate and up-to-date by reading our editorial policy.1 Syphilis; https://www.healthline.com/health/std/syphilis2 What Is Lattice Degeneration?; https://www.aao.org/eye-health/diseases/what-is-lattice-degeneration3 Ciliary body; https://medlineplus.gov/ency/article/002319.htm4 HOW TO USE THE DIRECT OPHTHALMOSCOPE; http://morancore.utah.edu/basic-ophthalmology-review/how-to-use-the-direct-ophthalmoscope/5 Toxoplasmosis; https://www.healthline.com/health/toxoplasmosis










































 Workout
Workout

 Meditation
Meditation



 Podcast
Podcast
 E-book
E-book