The Fast Facts
- Some major complications of Chronic Pancreatitis includes pain in abdomen, stone in the pancreatic duct (tube), diabetes and fat malabsorption later in life and in some cases leads to pancreatic cancer.
- An intense stomach ache or pain in the upper abdomen, radiating to the back and chest, lasting for hours to days, without relief, is typical of Acute Pancreatitis.
- According to one latest study, it has been found that survival rate is 70% in the last 10 years and 45% in the last 20 years.

What is Chronic Pancreatitis?
Pancreas is a digestive organ having both exocrine and endocrine function. It produces digestive juices and enzymes required for the digestion and absorption of fat, carbohydrate and protein as an exocrine organ. It transfers digestive juices and enzymes through a small duct to the duodenum. Its endocrine role is to secret two main hormones, namely Insulin and Glucagon to maintain glucose homeostasis. Chronic Pancreatitis is a condition in which inflammation of the pancreas takes place.
An intense stomach ache or pain in the upper abdomen, radiating to the back and chest, lasting for hours to days, without relief, is typical of Acute Pancreatitis. It could be chronic also, when inflammation develops with time and signs are difficult to recognize.
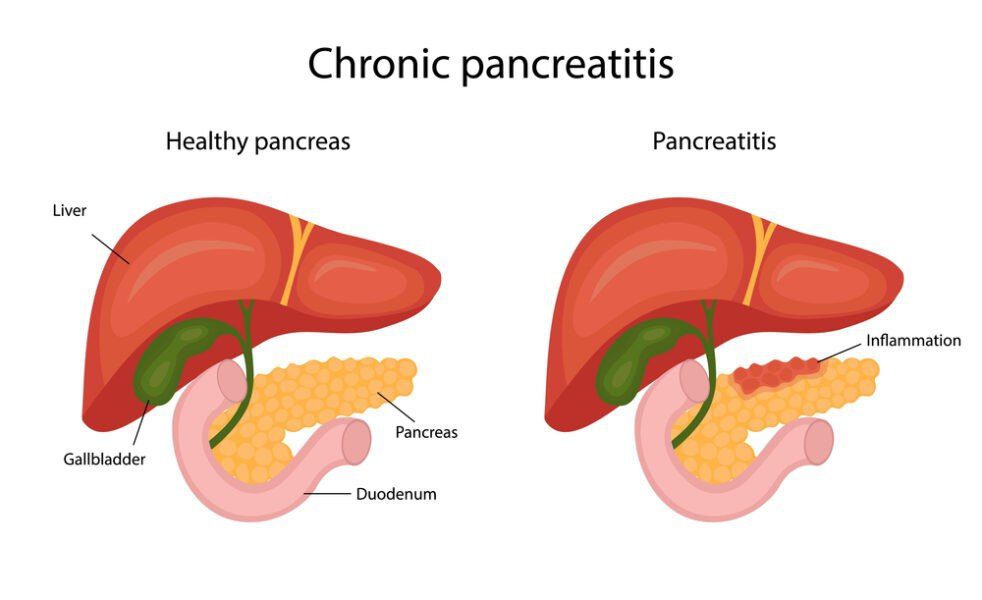
Chronic pancreatitis is a progressive inflammatory disease of the pancreas characterized by irreversible morphological changes which may cause pain and/or permanent loss of function. It may lead to the destruction of both the exocrine and endocrine tissues.(1)
Chronic Pancreatitis Life Expectancy.
Chronic pancreatitis is one of the serious condition. If it is left untreated it will cause fat malabsorption thereby, weight loss and other imbalance factors in the body. Thus, the patient is unable to lead a normal life. Even also chronic pancreatitis is not life threatening but many patient do not live long as the age grows.
According to one latest study, it has been found that survival rate is 70% in the last 10 years and 45% in the last 20 years. Therefore, overall it showed that the life expectancy in chronic pancreatitis created a standard mortality ratio 3.6.
Complications.
Tropical chronic pancreatitis (TCP) is a type of chronic pancreatitis generally seen in tropical countries like India. The cause of this is not fully known, but is commonly seen to effect children or young adults. Some major complications of Chronic Pancreatitis includes pain in abdomen, stone in the pancreatic duct (tube), diabetes and fat malabsorption later in life and in some cases leads to pancreatic cancer. TCP is more prevalent in southern India as compared to northern regions.
Causes of Chronic Pancreatitis.
Pancreatitis may have different etiology, but two most common causes are:
- Excessive alcohol consumption: Chronic heavy dose of alcohol causes chronic pancreatitis.
- Gall stone formation: People with acute pancreatitis mostly reported to have gall stones.
- Calcium deposits in the bile duct, increased triglyceride levels and bacterial or viral infection may be other probable causes for pancreatitis.
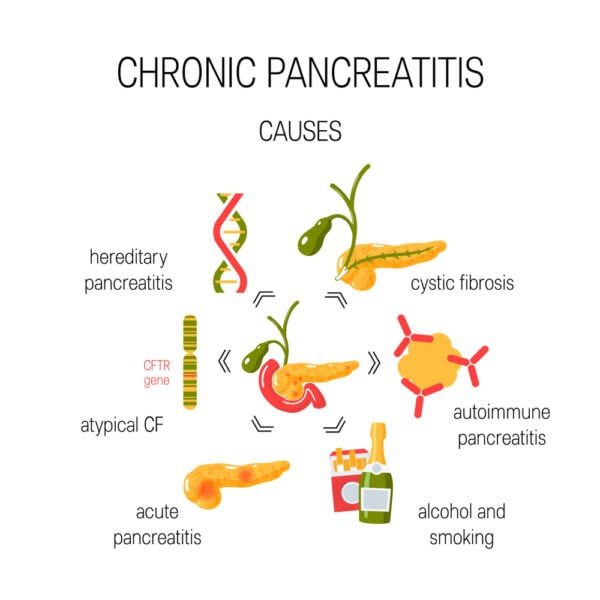
Main Causes.
The main causes of pancreatitis are:
- Chronic alcoholism.
- Gall Stones.
- Abdominal surgery or injury to the abdomen.
- Genetic.
- Increased calcium level in the blood.
- Infection.
- Smoking.
- Increased triglycerides.
- Abnormality in the structure of pancreas or pancreatic or bile duct.
- Certain drugs e.g. NSAIDS (non-steroidal anti-inflammatory drugs).
Signs and Symptoms.
Following are some common signs and symptoms of Chronic Pancreatitis;
- Upper abdominal pain.
- Nausea and vomiting.
- Fever.
- Bloating.
- Oily or bulky stool.
- Weight loss.
Nutritional Management.
Acute and chronic pancreatitis requires different nutritional approaches. The management of acute pancreatitis requires hospital admission. Chronic pancreatitis is largely treated by providing exogenous pancreatic enzymes, complete abstinence from alcohol and pain control.
Malnutrition may be commonly found in people with chronic pancreatitis. This can be majorly attributed to malabsorption and therefore nutrient depletion coupled with an increased metabolic activity due to severity of the disease.
Inability to meet up with the increased nutrient requirement may lead to weight loss, which is common feature in people suffering from chronic pancreatitis.(2) This could be because of insufficient calorie intake (due to pain or alcoholism) and malabsorption of nutrients.
Chronic Pancreatitis Diet.
While on enzyme therapy one can consume normal diet, however the following instructions need to be kept in mind:
- Complete avoidance of alcohol and smoking is recommended. Smoking may lead to the development of pancreatic cancer in a patient with pancreatitis.
- During chronic pancreatitis an increase in the resting energy expenditure has been reported. A high calorie diet has been thus recommended (about 35 kcal/ kg/ d).(3)
- Consumption of frequent small meals is recommended in order to ensure adequate intake and to decrease the demand for secretion of pancreatic enzymes and fluids.
- It is advised to not consume heavy meals in a single sitting. It increases the load on the pancreas for digestion leading to pain.
- Fat and protein malabsorption are common finding during chronic pancreatitis and which are commonly corrected by enzyme therapy (Lipase enzyme). About 4-5 tsp of oil/day can be consumed. It is recommended to not consume fried foods and foods rich in fats such as cheese, butter, margarine etc. This would worsen fat malabsorption in the body. Along with lipase enzyme therapy; about 30% of energy can be derived from fats (ESPEN guidelines, 2006).(4) Vegetable fats are better tolerated than animal sources of fat.
- If steatorrhea (fat excretion in stools) is present then the fat content of diet needs to be reduced. Medium chain triglycerides (MCT) are generally recommended during this condition. About 50g/d of MCT can be given. An amount exceeding this may be ketogenic and may also cause nausea, cramps and diarrhea.
- A deficiency of fat soluble vitamins vitamin A, D, E, K may be seen in patients with steatorrhea. It is important to assess the same and ensure adequate provision diet or supplementation. Water soluble forms these above mentioned vitamins may also considered.
- Deficiency of vitamin B12 may also be observed in people with chronic pancreatitis. This could be due to inadequate protease secretion by the pancreas which is essential for the release of vitamin B12 for absorption at the terminal ileum. If levels of vitamin B12 are low then supplementation of the same is recommended.
- Adequate protein consumption is vital in the diet as malnutrition and loss of lean body mass is a common finding in chronic pancreatitis. Up to 1-1.5g of protein/ kg body weight has been suggested as a safe (ESPEN guidelines 2006). Whole protein oral nutrition supplement couple with pancreatic enzyme can be provided. Whole proteins are not tolerated, hydrolyzed proteins and peptide formulations can be considered. It needs to be understood that palatability of peptide based formulations is low and therefore, compliance may be an issue.
- The diet needs to be low in its fiber content. Fiber may bind with available enzymes and lead to a reduced uptake of nutrients (ESPN guidelines, 2006).
- Antioxidants are seen to be low in the body of person suffering chronic pancreatitis. This may be due to malabsorption of nutrients or due to the increased stress load exerted by the illness in the body. Deficiency antioxidants may result in risk of greater pancreatic injury from relapse illness or progression to development of cancer. Antioxidant supplementation (vitamin C, A and E, selenium, L-methionine) under medical supervision is recommended. Antioxidant supplementation also helps in improving the quality of life by bringing about a reduction in the pain.
- Omega 3 fatty acids are known for their anti-inflammatory properties. Addition of omega 3 fats to diet in case of chronic pancreatitis is seen to be beneficial. They act anti-oxidants in body and help decrease the level of oxidative stress markers. Dietary sources of omega 3 include fish variety) and fish oils, walnuts and flax seeds.(5)
- Green tea also could be a good source of antioxidant. Studies show that consumption of green tea helps reduce pancreatic fibrosis.(6)
- Reduced bone mineral density resulting in osteopenia and osteoporosis to insufficient vitamin and mineral status is a common finding in patients with chronic pancreatitis. It is recommended to ensure consumption of minerals such as calcium and phosphorous in the diet, vitamin D and K supplementation is advised under medical supervision.(7)
- Zinc adequacy in diet is extremely important. Pancreas plays a major role in zinc homeostasis. Pancreatitis being inflammatory condition, zinc acts a potential antioxidant and helps in reducing the oxidative stress and reduces collagen deposition. Zinc is also known to be present in the pancreatic cells and helps in glucose metabolism. During pancreatitis, decline in the pancreatic zinc stores is possible which may also contribute to dysregulation of glycemic control.(8)
- If non-enteric coated enzyme tablets are being administered then foods that trigger acidity needs to be avoided.
Frequently Asked Questions.
Improper digestion lead to the accumulation of Ama (toxin that remain in body due to improper digestion) in the pancreatic cells which hamper insulin function. Therefore, adding lady’s finger in your diet helps to calm aggregated Vata and helps to cure digestion.
Yes, dry fruits can be given to the pancreatic patients but in minimal amount.
No, it is not suggested to eat foods rich in high carbohydrates during chronic pancreatitis. As it may affect insulin function because pancreatic patient cannot produce enough insulin that is required in conversion of glucose.
Bottom Line.
Therefore, chronic pancreatitis is marked by an increase in the resting energy expenditure leading to an increased nutritional requirement. Improper digestion and malabsorption of nutrients is a common finding in chronic pancreatitis.
So, complete avoidance of alcohol is mandatory. Most patients are put on enzyme therapy. Energy, Protein and Fat adequacy in the diet needs to be maintained. Antioxidant supplementation is essential as it aids in reducing the pain and in improvement of quality of life.
+14 Sources
Freaktofit has strict sourcing guidelines and relies on peer-reviewed studies, educational research institutes, and medical organizations. We avoid using tertiary references. You can learn more about how we ensure our content is accurate and up-to-date by reading our editorial policy.
- A proposal for a new clinical classification of chronic pancreatitis : https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2804657/
- Nutrition Treatment of Deficiency and Malnutrition in Chronic Pancreatitis: A Review : https://www.researchgate.net/publication/45629748_Nutrition_Treatment_of_Deficiency_and_Malnutrition_in_Chronic_Pancreatitis_A_Review
- Glucose Homeostasis : https://www.sciencedirect.com/topics/medicine-and-dentistry/glucose-homeostasis
- ESPEN guideline on clinical nutrition in acute and chronic pancreatitis; https://www.espen.org/files/ESPEN-Guidelines/ESPEN_guideline_on_Clinical_Nutrition_in_acute_and_chronic_pancreatitis.pdf
- Reduction of inflammation and chronic tissue damage by omega-3 fatty acids in fat-1 transgenic mice with pancreatitis : https://www.sciencedirect.com/science/article/pii/S0925443908001622
- Green tea and coffee intake and risk of pancreatic cancer in a large-scale, population-based cohort study in Japan (JPHC study) : https://www.researchgate.net/publication/5758972_Green_tea_and_coffee_intake_and_risk_of_pancreatic_cancer_in_a_large-scale_population-based_cohort_study_in_Japan_JPHC_study
- Proper Calcium Use: Vitamin K2 as a Promoter of Bone and Cardiovascular Health : https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4566462/
- Zinc in Specialized Secretory Tissues: Roles in the Pancreas, Prostate, and Mammary Gland : https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3065755/
- Tropical chronic pancreatitis : https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1742869/
- Enzyme therapy: a forerunner in catalyzing a healthy society? : https://pubmed.ncbi.nlm.nih.gov/32597245/
- Steatorrhea (Fatty Stool) : https://www.healthline.com/health/steatorrhea
- Amatoxin : https://www.sciencedirect.com/topics/agricultural-and-biological-sciences/amatoxin
- Vata Diet: All You Need To Know About This Dosha And A Regime To Pacify The Imbalance : https://www.netmeds.com/health-library/post/vata-diet-all-you-need-to-know-about-this-dosha-and-a-regime-to-pacify-the-imbalance
- Chronic Pancreatitis : https://www.healthline.com/health/chronic-pancreatitis#







































 Workout
Workout

 Meditation
Meditation



 Podcast
Podcast
 E-book
E-book