The Fast Facts
- In the earliest stages, the tumor is small and confined to the liver, and overall liver function is typically well preserved.
- With appropriate management and expert supervision, patients in the intermediate stage can maintain a good quality of life while effectively controlling disease progression.
- Surgical resection is often recommended if the tumor can be safely removed and the remaining liver tissue is healthy.

Liver cancer management has progressed significantly over the past decade, offering patients more advanced treatment options and improved survival outcomes. With early diagnosis, personalized therapies, and coordinated multidisciplinary care, many individuals now experience a better quality of life throughout treatment. Understanding how liver cancer treatment varies by disease stage allows patients and families to make informed, confident decisions. This guide clearly explains stage-wise liver cancer management while highlighting the importance of specialized care.
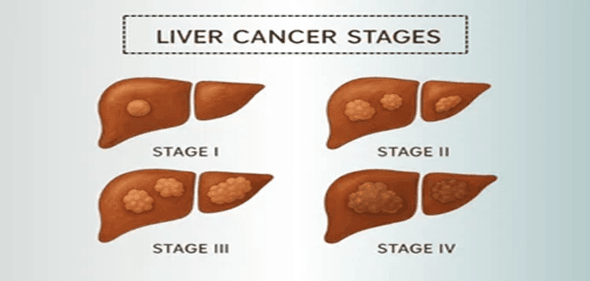
Stage 0 and Stage A (Early-Stage Liver Cancer)
In the earliest stages, the tumor is small and confined to the liver, and overall liver function is typically well preserved. At this point, treatment focuses on achieving a cure whenever possible.
Surgical resection is often recommended if the tumor can be safely removed and the remaining liver tissue is healthy. Liver transplantation is another highly effective treatment, especially for patients who have both liver cancer and advanced cirrhosis. By replacing the diseased liver entirely, transplantation eliminates both the tumor and the underlying liver damage, significantly improving long-term survival chances.
Minimally invasive treatments also play a crucial role in early-stage liver cancer management. Procedures such as radiofrequency ablation and microwave ablation destroy cancer cells using targeted heat therapy. These advanced procedures are typically performed by an experienced Interventional Radiologist, who uses image-guided technology to locate and treat the tumor precisely. This specialized approach reduces damage to surrounding healthy tissue and promotes faster recovery compared to traditional open surgery.
Early-stage liver cancer management offers the best opportunity for long-term survival, particularly when combined with consistent follow-up care and healthy lifestyle adjustments.
Stage B (Intermediate-Stage Liver Cancer)
In intermediate-stage liver cancer, multiple tumors may be present within the liver, but the disease has not spread to distant organs. Liver function often remains stable, allowing physicians to implement active treatment strategies aimed at slowing tumor growth.
One of the most commonly used treatments at this stage is transarterial chemoembolization (TACE). This procedure delivers chemotherapy directly to the tumor while blocking its blood supply, effectively limiting cancer growth. Another advanced therapy is transarterial radioembolization (TARE), which uses radioactive particles to target and destroy cancer cells internally.
Many patients seek treatment at an International Hospital that offers comprehensive liver cancer programs. These specialized centers typically provide advanced imaging technologies, multidisciplinary tumor boards, and access to the latest treatment innovations. Receiving care in such a facility enhances treatment precision and ensures that patients benefit from globally recognized standards of cancer care.
With appropriate management and expert supervision, patients in the intermediate stage can maintain a good quality of life while effectively controlling disease progression.
Stage C (Advanced-Stage Liver Cancer)
Advanced-stage liver cancer develops when the tumor invades major blood vessels, lymph nodes, or spreads beyond the liver. Although this stage presents greater challenges, significant advancements in systemic therapies have improved outcomes.
Targeted therapy involves medications that block specific pathways cancer cells use to grow and spread. Drugs such as sorafenib and lenvatinib have demonstrated improved survival in many patients. Immunotherapy has further transformed advanced liver cancer treatment by strengthening the body’s immune response against cancer cells.
Combination therapies, particularly those integrating immunotherapy with targeted drugs, are increasingly used and have shown promising results. Even in advanced stages, personalized treatment plans can help extend survival and manage symptoms effectively.
Stage D (End-Stage Liver Cancer)
In end-stage liver cancer, liver function becomes severely impaired, and the disease may be widespread. At this stage, treatment primarily focuses on supportive and palliative care.
The main goal is to relieve symptoms, manage pain, provide nutritional support, and maintain patient comfort and dignity. Emotional and psychological support also become essential component of care. While curative treatments may no longer be possible, compassionate medical management significantly improves the quality of life for both patients and their families.
The Importance of a Multidisciplinary Approach
Effective stage-wise liver cancer management requires close collaboration among hepatologists, oncologists, surgeons, radiologists, and palliative care specialists. Each patient’s treatment plan must be individualized based on tumor stage, liver function, overall health, and personal preferences.
Regular follow-up visits, imaging studies, and laboratory tests are vital to monitor treatment response and detect recurrence early. Ongoing communication between the healthcare team and the patient ensures that care remains aligned with treatment goals and evolving medical needs.
Moving Forward with Confidence
Modern advancements in liver cancer management continue to bring renewed hope. From curative treatments in early stages to innovative systemic therapies in advanced cases, options are expanding every year. Early diagnosis, access to specialized care, and guidance from experienced professionals play a crucial role in achieving better outcomes.
By understanding stage-wise treatment strategies and seeking expert care when needed, patients can move forward with clarity, confidence, and optimism. With continued research and medical innovation, the future of liver cancer care remains increasingly promising.
Frequently Asked Questions.
1 What is the best treatment for early-stage liver cancer?
Early-stage liver cancer is often treated with surgical resection, liver transplantation, or ablation therapy. The best option depends on tumor size, liver function, and overall patient health. When diagnosed early, treatment can be potentially curative.
2 Who performs minimally invasive liver cancer treatments?
Minimally invasive procedures such as radiofrequency ablation, TACE, and TARE are typically performed by a specialized Interventional Radiologist using advanced imaging guidance to precisely target tumors.
3 Can liver cancer be cured?
Liver cancer can be cured if detected at an early stage and treated promptly with surgery or transplantation. In later stages, treatments focus on controlling disease progression and improving survival.
Conclusion
Stage-wise liver cancer management provides a structured and personalized approach to treatment, ensuring that each patient receives care tailored to the severity of the disease and their overall liver function. From potentially curative options in early stages to advanced systemic therapies and supportive care in later stages, modern medicine offers multiple pathways to improve survival and maintain quality of life.










































 Workout
Workout

 Meditation
Meditation



 Podcast
Podcast
 E-book
E-book